Hundreds of women in the U.S. die each year from complications related to pregnancy and childbirth. Pregnant women with COVID-19 are more likely to experience complications.
The GAO analyzed CDC data and found:
- Maternal deaths increased during the pandemic compared to 2018 and 2019
- COVID-19 contributed to 25% of maternal deaths in 2020 and 2021
- The maternal death rate for Black or African-American women was disproportionally higher compared to White and Hispanic or Latina women
Health and Human Services officials and stakeholders we interviewed said the pandemic worsened factors contributing to maternal health disparities, like access to care.
What GAO found:
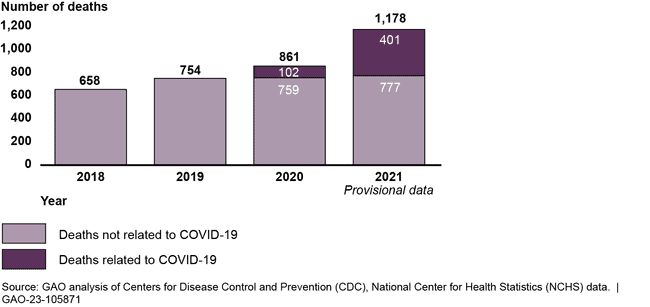
Each year in the U.S., hundreds of women die from complications related to pregnancy and childbirth—known as maternal death. GAO’s analysis of Centers for Disease Control and Prevention (CDC) data shows that maternal deaths increased during the COVID-19 pandemic. Further, the data show that COVID-19 was a contributing factor in one quarter of all maternal deaths in 2020 and 2021 combined.
CDC data also show racial and ethnic disparities in the rate of maternal deaths per 100,000 live births per year. For example:
- The maternal death rate for Black or African-American (not Hispanic or Latina) women was 44.0 per 100,000 live births in 2019, then increased to 55.3 in 2020, and 68.9 in 2021. In contrast, White (not Hispanic or Latina) women had death rates of 17.9, 19.1, and 26.1, respectively.
- The maternal death rate for Hispanic or Latina women was lower (12.6) compared with White (not Hispanic or Latina) women (17.9) in 2019, but increased significantly during the pandemic in 2020 (18.2) and 2021 (27.5).
Disparities in other adverse outcomes, such as preterm and low birthweight births, persisted for Black or African-American (not Hispanic or Latina) women, according to GAO analysis of CDC data.
Stakeholders and Department of Health and Human Services (HHS) officials told GAO that the pandemic exacerbated the effects of social determinants of health—factors such as access to care, transportation, or technology; living environment; and employment—on maternal health disparities. For example, service reductions in public transportation and child care worsened existing barriers to accessing care. In addition, stakeholders and officials said the pandemic highlighted the effect racism has on maternal health. For example, physiological changes caused by chronic stress can increase the risk of maternal death, as well as severe illness from COVID-19.
The full GAO report can be downloaded here: https://www.gao.gov/products/gao-23-105871