Introduction

Understanding Chronic Care Management (CCM) is crucial for medical staff and healthcare providers as it offers a detailed care plan and coordination services to Medicare beneficiaries with multiple chronic conditions. CCM not only improves patient outcomes but also reduces healthcare costs, increases patient satisfaction, and aids in better coordination of care.
Below, we will delve deeper into the world of CCM – from eligibility criteria to enrollment processes, components of CCM, care team and providers involved in the process, challenges that come
along with it, technology used in CCM implementation, tips for successful management and the value it brings to patients’ health.
What is Chronic Care Management (CCM)?
Chronic Care Management (CCM) refers to non-face-to-face services provided by medical professionals to patients with multiple chronic conditions, aimed at improving the quality of care and helping
them manage their conditions more effectively.
Definition and Overview
In today’s complex healthcare world, managing chronic conditions is a top priority for medical professionals.
Chronic Care Management (CCM) services have emerged as an important way to provide non-face-to-face care to Medicare beneficiaries with multiple chronic conditions.
But what exactly is CCM, and who can benefit from it? Following, we take a deep dive into understanding chronic care management, including its definition, benefits, components of care management services and eligibility requirements. CCM can improve patient outcomes and reduce healthcare costs while increasing satisfaction among patients and providers alike.
Importance of CCM in Healthcare
Chronic Care Management (CCM) is an essential approach to healthcare that helps patients manage their chronic conditions, including those with multiple serious ailments. CCM services are designed to provide comprehensive care planning, medication management, and coordination of care between visits for improved outcomes. Healthcare providers can bill Medicare for these non-face-to-face services, which not only benefits patients but also provides them with additional revenue streams.
The importance of CCM in healthcare cannot be overstated. It helps mitigate the risks associated with multiple chronic conditions, reduces hospitalizations and emergency department visits while improving patient satisfaction with their care. Providing this continuity of care minimizes the need for costly interventions like surgeries or other invasive treatments that may adversely affect a patient’s health outcome.
Moreover, insurance companies are beginning to recognize the value of CCM in reducing healthcare costs while keeping patients healthier and happier by investing more resources into it. These programs empower patients to take charge of their health by working closely with their primary care teams to achieve optimal health goals through active engagement, communications utilizing community resources & self-management techniques such as telemedicine technology, or use of mobile apps that prevent infectious diseases from spreading among high-risk populations.
Who Can Benefit From CCM?
CCM services can benefit Medicare beneficiaries who suffer from two or more chronic conditions, such as diabetes, hypertension, and heart disease. These individuals require additional resources and support to manage their health effectively between face-to-face appointments. CCM provides opportunities for healthcare professionals to track these patients’ health goals closely, provide care coordination across multiple providers, and help patients navigate the healthcare system.
See further information in the CMS CCM FAQ.
Moreover, CCM benefits those patients who are at significant risk of developing a new illness or experiencing worsening symptoms due to their chronic conditions. Patients with low-income status may also be eligible for additional resources through Medicaid services that supplement traditional Medicare coverage. By identifying patients early on in the course of their illness and initiating CCM services promptly, healthcare professionals can reduce hospitalizations related to avoidable complications
arising from chronic diseases.
Ultimately, all parties involved benefit from successful Chronic Care Management programs – insurance companies realize lower costs associated with preventable hospitalizations; physicians reap financial rewards for providing valuable care outside standard office visits; and most importantly – engaged patient experience improved overall health outcomes.
Benefits of Chronic Care Management
Chronic Care Management (CCM) provides numerous benefits, including improved patient outcomes, increased patient satisfaction, reduced healthcare costs, and better coordination of care.

One of the primary goals of Chronic Care Management (CCM) services is to improve patient outcomes. Studies have shown that patients who participate in CCM experience better health outcomes and fewer preventable hospitalizations. Through comprehensive care planning, medication management,
remote patient monitoring, and other interventions, patients are empowered to take control of their own health.
In addition to improved physical health outcomes, CCM contributes significantly to mental and emotional well-being. Patients who receive regular support from their care team are more likely to adhere to treatment plans and be satisfied with their overall healthcare experiences. This sense of partnership can lead to increased confidence in managing chronic conditions and ultimately result in better long-term health outcomes.
Increased Satisfaction
When patients receive ongoing support and engage in proactive care planning with their providers, they often feel more heard, understood, and empowered to make positive changes in their health.
Studies have shown that patients who participate in chronic care management programs report higher levels of satisfaction with their healthcare experience. This can lead to improved access
to healthcare services, better adherence to treatment plans, and ultimately better clinical outcomes.
Providers also report higher levels of satisfaction when implementing chronic care management models. By empowering patients to take an active role in their own care and providing ongoing support
through a collaborative team approach, providers are able to improve the quality of care provided while reducing administrative burden and burnout.
Reduced Healthcare Costs
One of the key benefits of Chronic Care Management (CCM) is its ability to reduce overall healthcare costs. By providing timely and coordinated care, CCM can help prevent unnecessary hospital admissions and emergency room visits, which in turn significantly cuts down healthcare expenses.
Research shows that CCM not only reduces healthcare costs but yields significant savings as well. A study conducted by CMS revealed that patients who received CCM services had a 5.6% reduction in total Medicare expenditures per beneficiary per quarter compared to those who didn’t receive CCM services.
Better Coordination of Care
Better coordination of care is at the heart of chronic care management. Patients with multiple chronic conditions often receive care from a variety of healthcare providers, making it challenging to ensure that all aspects of their health are appropriately addressed. CCM aims to improve this by providing a comprehensive care plan that considers all aspects of the patient’s health, including their mental and emotional well-being.
CCM can also help reduce hospital readmissions and emergency department visits by facilitating timely
interventions among patients. This includes medication adjustments, symptom management, and lifestyle modifications. The result is improved quality of life for patients with chronic conditions.
Eligibility and Enrollment in Chronic Care Management
Criteria For Eligibility

To be eligible for Chronic Care Management, patients must have two or more chronic conditions that are expected to last at least 12 months. These conditions could include arthritis, hypertension, diabetes, and other illnesses. This program is designed to provide care coordination services to individuals with complex medical needs.
Medicare beneficiaries may qualify for CCM services if they have two or more serious chronic conditions expected to last a year or longer. To confirm eligibility, providers should review the patient’s medical history and conduct a comprehensive wellness visit. Once confirmed as qualified for CCM services, patients can benefit from monthly check-ins by their healthcare team.
With over 133 million Americans living with at least one chronic disease,
there is no shortage of potential candidates who could benefit from Chronic Care Management. Providers play an important role in helping their patients enroll in this program and receive the additional support needed to manage their health effectively.
Enrollment Process and Requirements
The enrollment process for Chronic Care Management (CCM) involves several steps that aim to ensure patients receive the best care possible. Firstly, healthcare professionals need to identify and recruit eligible patients who have two or more serious chronic conditions that are expected to last for at least a year. They then develop a comprehensive care plan tailored to each patient’s health goals and needs.
To provide CCM services, healthcare providers must form a care team consisting of multiple disciplines, including registered nurses, clinical nurse specialists, physician assistants, and certified nurse midwives. The team will collaborate with specialized providers and services as needed in a coordinated approach to patient care.
Patients must give their consent before enrolling in the CCM program. It is essential to involve patients actively throughout the enrollment process by informing them of the benefits of CCM services and empowering them through regular follow-ups, open communication with their care team, self-management education sessions, and utilizing community resources.
Medicare CCM Reimbursement
Medicare offers reimbursement for Chronic Care Management (CCM) services to eligible healthcare providers. These services help manage multiple chronic conditions of Medicare beneficiaries between physician visits. The Medicare Physician Fee includes payable service codes for CCM, and providers can bill separately for these services.
To be eligible for reimbursement, patients must have two or more chronic conditions that are expected to last at least a year or until the patient’s death. Additionally, patients must sign consent forms before receiving CCM services from their care team members and agree to participate actively in their care plan.
The reimbursement rates vary based on the type of provider who bills for these services regularly. For example, primary care providers may receive higher reimbursements compared to specialists providing these services in addition to their regular practice.
Components of Chronic Care Management

Chronic Care Management includes comprehensive care planning, medication management, communication, and education, as well as remote patient monitoring devices. Discover why each of
these components is essential to managing chronic conditions effectively by reading on.
Comprehensive Care Planning
Comprehensive care planning is a critical component of Chronic Care Management (CCM). It involves developing and implementing a personalized care plan that addresses the patient’s unique needs, goals, and preferences. The comprehensive care plan should include information on the patient’s chronic conditions, medication management strategies, preventive measures, and any other relevant health information.
The development of a comprehensive care plan requires input from the patient’s entire healthcare team to ensure that every aspect of their health is considered. This includes primary care providers, specialists like clinical nurse specialists or certified nurse midwives who are involved in managing specific chronic conditions. This approach to collaborative goal setting among patients’ healthcare professionals
has been shown to improve outcomes.
One key benefit of comprehensive care planning is better coordination of care between different healthcare providers. By having all information about a patient’s health status in one place,
everyone involved can make informed decisions about their treatment plans.
Additionally, by identifying potential areas for improvement early on in the
process through well-constructed documentation, more efficient decision-making
for interventions can be made earlier in treatment. Ultimately creating efficiencies leading to improved outcomes for patients with multiple chronic conditions often seen where CCM services are delivered efficiently, including specific populations such as Alzheimer’s disease across nursing homes and assisted living facilities.
Medication Management
Medication management is a critical part of chronic care management programs that aim to improve patient outcomes for those with multiple chronic conditions. The safe and effective use of
medications can help reduce hospitalizations, prevent emergency room visits, and ensure patients take their medications as prescribed. Chronic care management services often include medication reconciliation, prescription refills, reviewing potential drug interactions, monitoring for side effects, and ensuring adherence to medication regimens.
One significant benefit of including medication management in chronic care programs is the increased collaboration between healthcare providers. By creating a comprehensive care plan that includes medication management strategies, all members of the patient’s care team can work together more effectively across different settings. This collaborative approach allows for better coordination and reduces the risk of errors in prescribing or taking medications.
Using technology such as electronic health records (EHRs) and remote patient monitoring devices can also enhance medication management practices in chronic care settings. Providers can easily access up-to-date information on a patient’s medical history and current conditions through EHRs. Remote monitoring devices allow healthcare professionals to track changes in vital signs or symptoms related to medication use remotely, allowing early intervention if necessary. By implementing best practices in medication management within chronic care programs, patients with multiple chronic conditions may experience improved quality of life while reducing overall healthcare costs.
Remote Patient Monitoring Devices
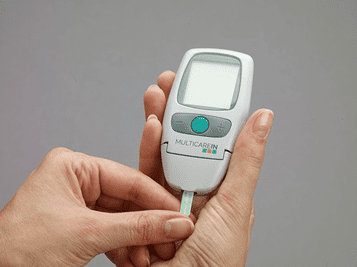
Remote patient monitoring devices are essential tools in chronic care management that allow healthcare providers to monitor patients’ health status remotely. This type of technology involves the use of devices such as wearables, sensors, and mobile apps that collect real-time data about a patient’s vitals and symptoms. With remote patient monitoring, physicians can continuously track the progress of their patients and intervene before complications occur.
By having access to timely data on essential parameters such as blood pressure or glucose levels, healthcare providers can take early interventions to prevent acute exacerbations, which may lead to emergency room admissions. Patients with chronic diseases would
otherwise need frequent check-ups and hospital visits.
Care Team and Providers for Chronic Care Management
The success of Chronic Care Management (CCM) relies heavily on the collaboration between primary care providers and specialized providers, including clinical nurse specialists, certified nurse midwives, nurse practitioners, physician assistants, and other members of the patient’s care team.
Roles of Primary Care Providers and Care Teams

Primary care providers and their care teams play a significant role in Chronic Care Management (CCM). They provide the foundation for coordinating patient care within a medical home setting. The primary care provider is responsible for overseeing all aspects of the patient’s health, including working with specialists and other healthcare professionals to ensure that patients receive comprehensive care.
The primary care team consists of clinical staff members such as registered nurses, nurse practitioners, physician assistants, and certified nurse midwives who work together with the primary care provider to provide quality chronic disease management services regularly. Each person on the team has specific responsibilities through patient engagement and identifying patients eligible for CCM services.
Roles of Specialized Providers and Services
Specialized providers and services play instrumental roles in Chronic Care Management (CCM). Clinical Nurse Specialists, Certified Nurse Midwives, Nurse Practitioners, and Physician Assistants can all initiate CCM services while working collaboratively with the patient’s care team. These providers aid in identifying patients who meet CCM eligibility criteria by using Electronic Health Records (EHRs) to review patient charts for two or more chronic conditions.
Additionally, behavioral health integration is critical because it helps identify patients with significant risk exposure to infectious diseases such as Alzheimer’s disease or other related disorders. Patients’ caregivers must also receive appropriate education on how best to support themselves and their loved ones.
CCM Technology and Tools
CCM Technology and Tools include Electronic Health Records (EHRs), patient portals, telehealth services, mobile health applications, and remote patient monitoring devices to improve communication, coordination of care, and patient outcomes.
Electronic Health Records (EHRs)
Electronic Health Records (EHRs) are a vital tool in Chronic Care Management (CCM). These records allow for the efficient and accurate tracking of patient health data, medication management,
and care coordination. EHRs also facilitate collaboration between healthcare
providers by providing real-time access to patient information across different
medical practices and care settings.
Open source Electronic Health Records can be especially beneficial for safety-net medical settings where patients may not have consistent access to healthcare or insurance coverage. Additionally, rural healthcare providers can use EHRs to identify which patients qualify for CCM services prior to their visit.
Patient Portals and Telehealth Services
Patient portals and telehealth services are essential tools for Chronic Care Management (CCM), allowing patients to access their medical information remotely. These technological advancements give patients convenient access to important health data, including lab results, medication lists, and appointment schedules. In addition, telehealth services allow remote clinical communication between the
patient and the healthcare provider.
Patients with chronic conditions can significantly benefit from these CCM technologies since they provide a means of monitoring health status remotely. Monitoring daily vitals using wearable
biosensors or other connected devices enables timely intervention should any
negative changes occur in a patient’s condition.
Electronic Health Records (EHRs) play a vital role in connecting all members of the care team by providing real-time updates on patient care plans, treatment goals, and medication history.
Integrated EHR tools help facilitate communication between providers and
enhance the coordination of care for patients with complex conditions.
Mobile Health Applications
Mobile health applications have become an essential tool in supporting the Chronic Care Model (CCM) for patients with chronic conditions. These apps provide patients with access to personalized care plans, medication reminders, and other self-management tools. A recent study found that mobile app use was associated with significant improvements in treatment adherence, medication management, and disease self-management among patients with multiple chronic conditions.
Remote Patient Monitoring Devices
Remote patient monitoring (RPM) devices are a vital component of chronic care management. These devices allow for real-time tracking and monitoring of a patient’s health status, enabling
healthcare providers to intervene immediately when necessary. RPM programs gather standard physiological information such as vital signs, weight, blood pressure, and heart rate. With this data in hand, healthcare providers can create personalized care plans that cater to the specific needs of the patient.
Challenges and Opportunities in CCM
While the benefits of the Chronic Care Management model are plentiful, there are still challenges and opportunities that come with its implementation.
Barriers to CCM Adoption and Implementation
Despite the benefits of chronic care management (CCM) services, there are barriers to their adoption and implementation in healthcare. These challenges include complicated coding, burdensome
paperwork, and low reimbursement rates for providers. The high complexity of CCM codes makes it challenging for providers to bill correctly, leading to fewer reimbursements from insurance companies. Another barrier is the adoption of the care manager role by primary care physicians (PCPs). PCPs
may not have adequate training or resources to manage patients with complex conditions effectively.
Tips for Successful Chronic Care Management
Active patient participation, open communication with the care team, regular follow-ups, empowering patients and caregivers, and utilizing community resources are all essential components of
successful chronic care management. Read on to learn more about how these tips can help improve outcomes for patients with chronic conditions.
Active Patient Participation
Active patient participation is an essential component of successful chronic care management (CCM). Patients with chronic conditions who are engaged in their own care tend to have better health
outcomes and increased satisfaction with their medical treatment. For patients with multiple chronic conditions, understanding their role and responsibilities in managing their health can be a critical factor in achieving positive results.
To encourage active patient participation, healthcare providers should make sure that patients are fully informed about the benefits of CCM as well as the specific details of their individual care plan. Patients must also feel empowered to ask questions and express concerns so they can work collaboratively with members of their care team to achieve optimal health outcomes.
In addition, utilizing community resources such as support groups or disease-specific organizations may help cultivate a sense of responsibility for one’s own overall well-being.
Empowering patients through education on self-management and providing tailored tools for tracking symptoms or medication compliance could also reinforce engagement levels among those receiving CCM services.
Regular Follow-ups
Regular follow-ups are essential for successful chronic care management. Patients with multiple chronic conditions require ongoing support and coordination from their healthcare providers to manage their health effectively. Regular check-ins with patients can help identify any changes in their health status or medication needs early on, preventing a decline in their condition that may lead to hospitalization.
Regular communication between the patient and care team helps build trust and engagement. The Chronic Care Model emphasizes the importance of continuous care planning, which includes regular assessments of patients’ clinical status and progress towards treatment goals.
Empowering Patients and Caregivers
Empowering patients and caregivers is a crucial aspect of any chronic care management program. Patients who feel empowered are more engaged in their healthcare, take better care of themselves, and are less likely to be readmitted to the hospital. Chronic Care Managers can help patients establish healthcare goals and identify barriers that may be hindering them. By educating patients on how to manage their chronic conditions, they can become an active participant in their own healthcare.
Patients with multiple chronic conditions often face complex medical needs that can lead to feelings of frustration or anxiety. By empowering these patients, they can become more resilient when managing their various illnesses.
The Value of Chronic Care Management in Improving Patient Outcomes and Healthcare Efficiency
Chronic Care Management is an essential service that provides comprehensive care planning, medication management, and communication for patients with multiple chronic conditions. By improving patient outcomes and satisfaction while reducing healthcare costs, CCM offers many benefits to both providers and their patients.
With the support of qualified medical staff and advanced technologies like electronic health records and remote patient monitoring devices, CCM can help achieve better coordination of care among
different providers while empowering patients to take control of their own health. As such, it’s clear that investing in Chronic Care Management is a valuable way to improve healthcare efficiency across the board.